Medication
adherence
for adults 65+
DoseCare is a medication management iOS app built around one core unmet need — confirmation. Designed from 9 user interviews and 129 research notes.

DoseCare is a medication management iOS app built around one core unmet need — confirmation. Designed from 9 user interviews and 129 research notes.

Older adults managing multiple daily medications face a problem that goes beyond scheduling. The challenge is often not remembering to take medication — it's remembering whether it was already taken. Existing reminder apps send alerts but offer no confirmation, no recovery from uncertainty, and no way to prove adherence.
Apps like Perx require complex manual prescription entry that many 65+ users cannot complete independently. This creates a reliance on family members at the very first step — before the product has delivered any value.
“How might we design a medication experience that helps older adults stay independent while making adherence more visible, understandable, and trustworthy?”
Semi-structured interviews with patients and caregivers, secondary research on the doctor perspective, and affinity mapping with tag-based synthesis. 129 notes were cleaned, tagged, and grouped into themes around uncertainty, overload, reminder fatigue, and weak support loops.
The core finding shifted the product direction: adherence is not a scheduling problem — it is a confidence problem.
“I've taken so many pills I can't always remember if I already took today's.”
“I call her every day just to make sure she's taken her medication. I can't always tell if she actually has.”
9 interviews · 129 notes · affinity mapping → 5 findings
Each decision prioritized reducing friction over adding features.
Decision 01 — Home Screen
Decision 02 — Dose Confirmation
Decision 03 — Scan to Add
Decision 04 — Smarter Notifications
Decision 05 — Medication Detail
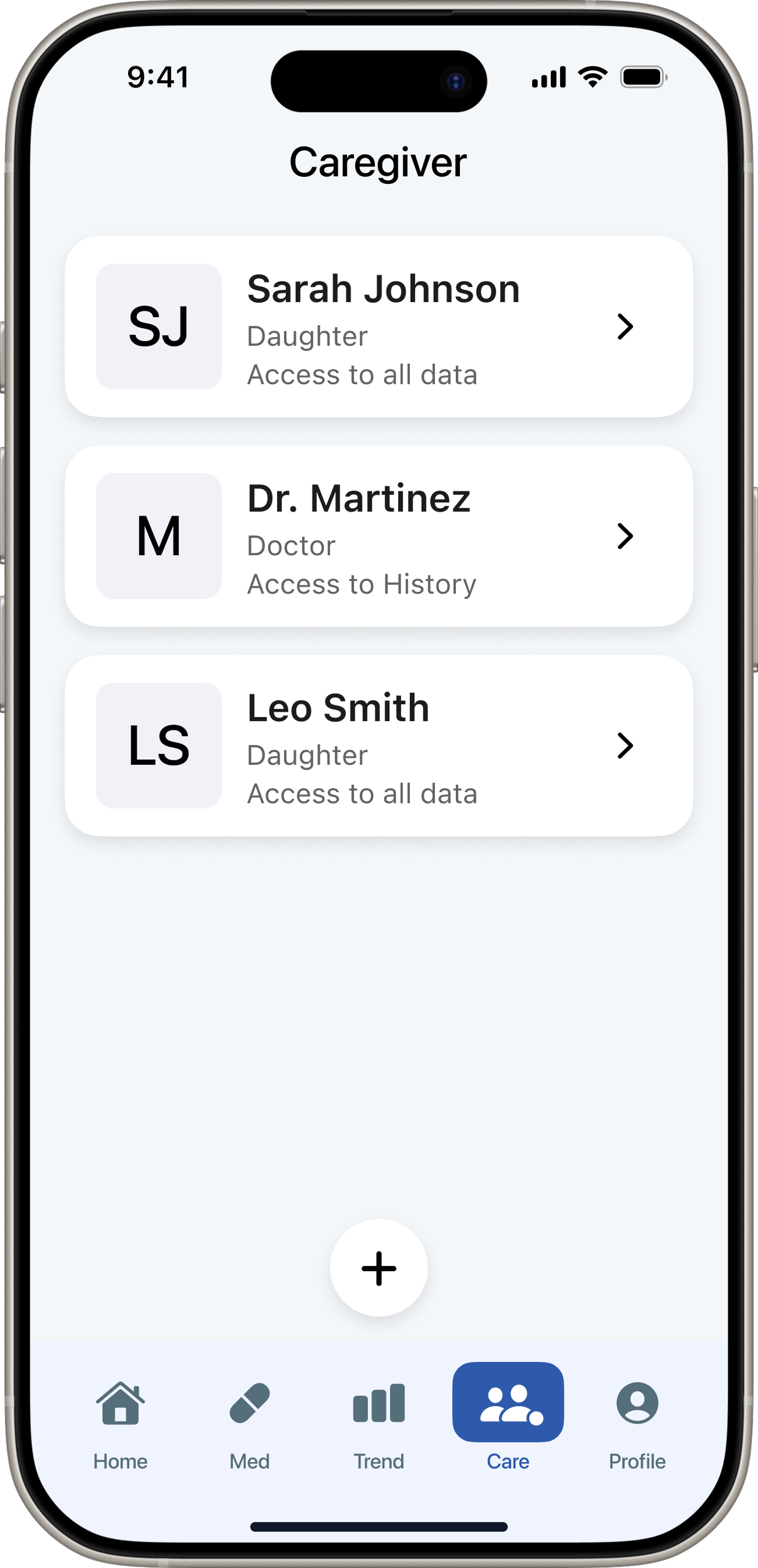
Decision 06 — Caregiver Visibility
Derived directly from research insights. Each design decision was evaluated against these principles.
Built directly from design decisions. Usability testing revealed where these assumptions broke down.

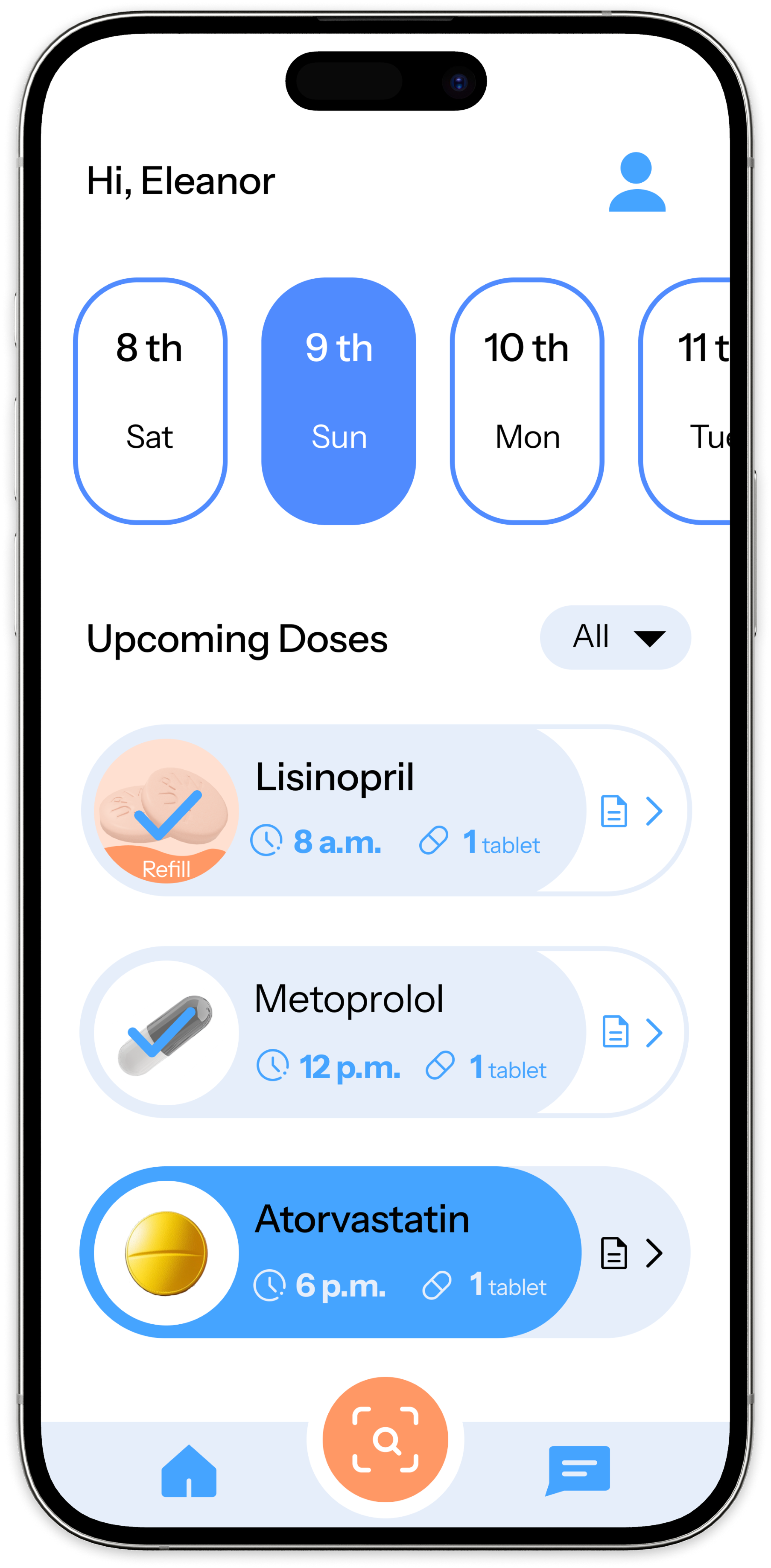

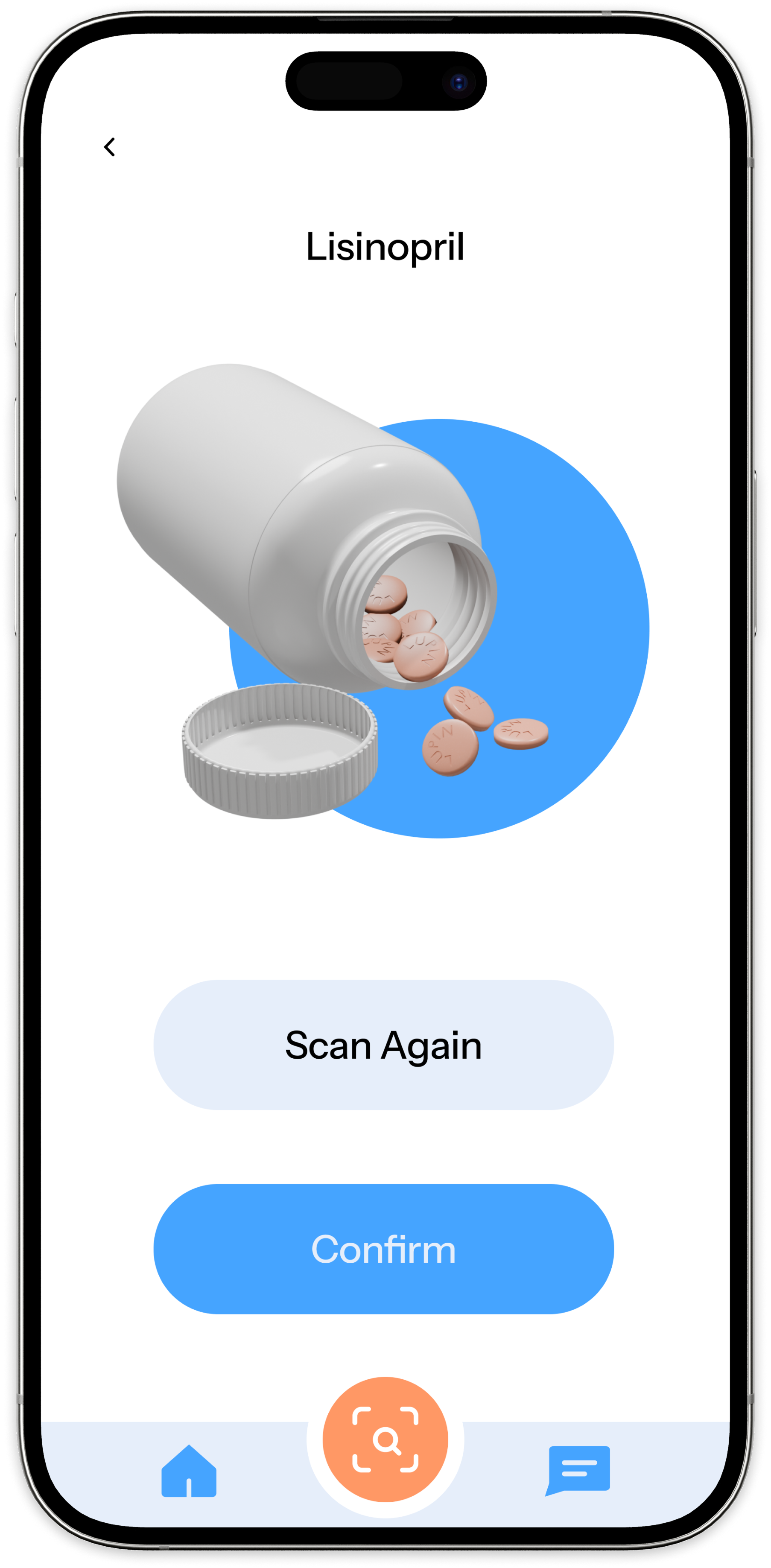
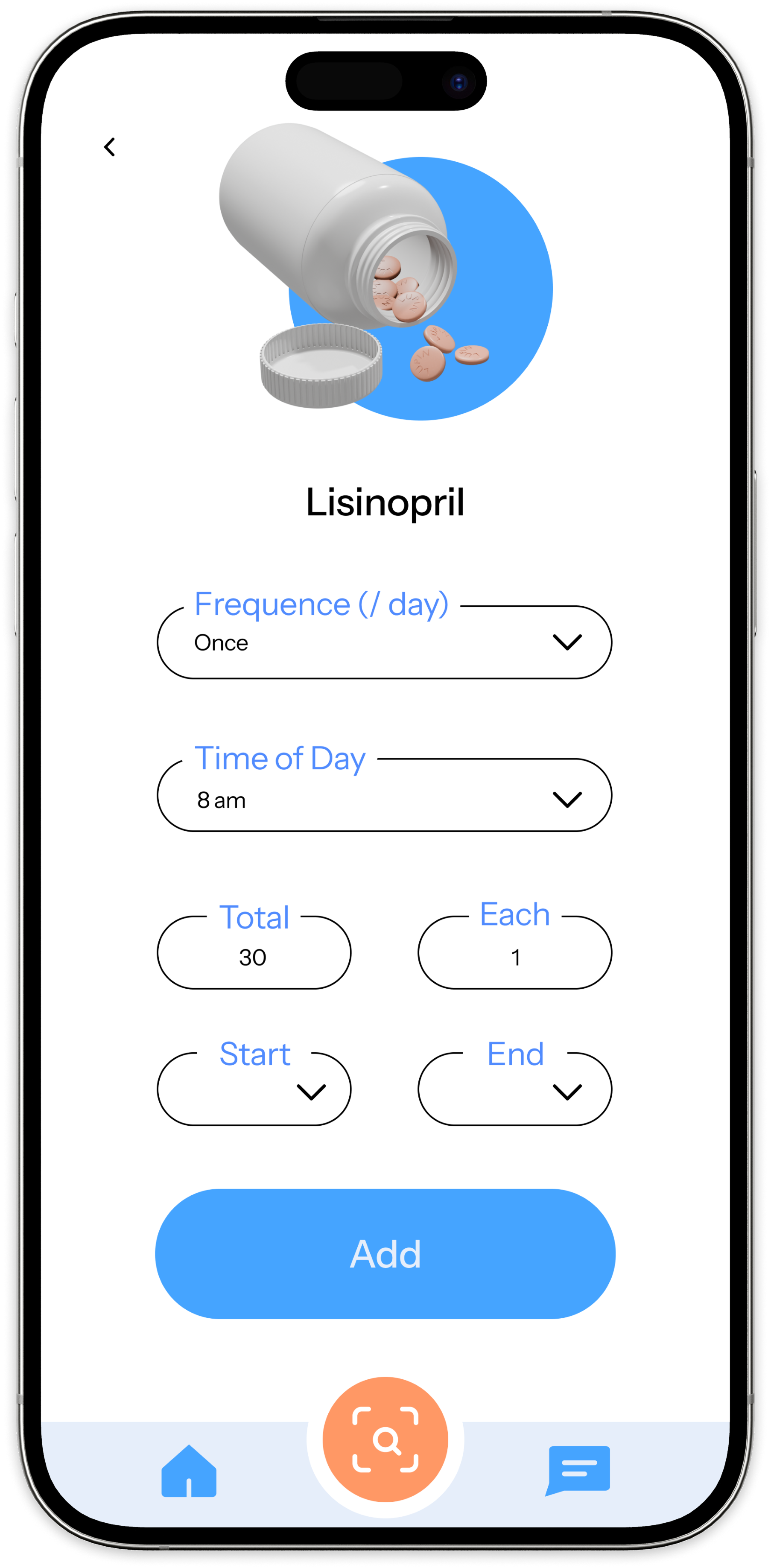
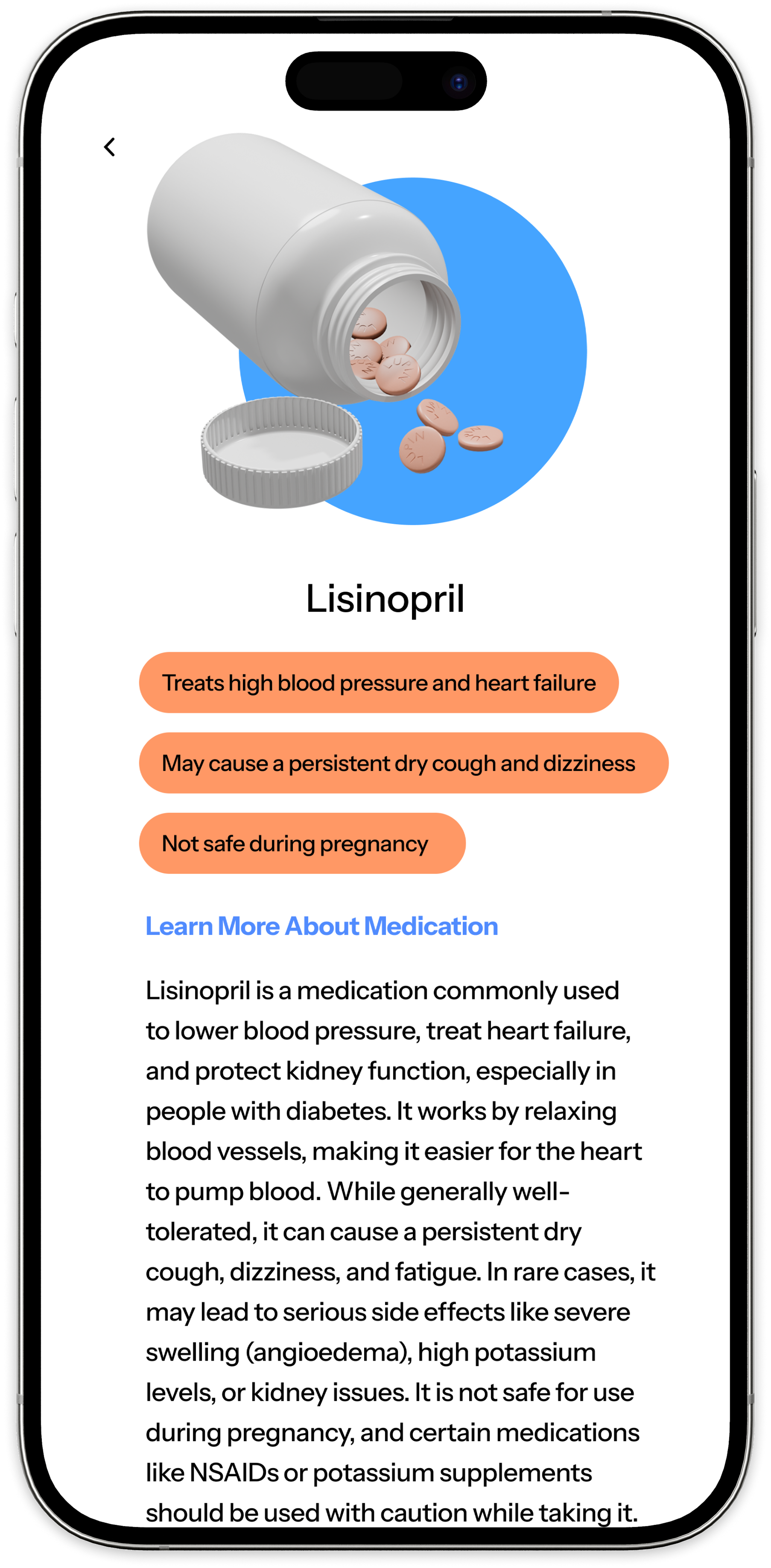
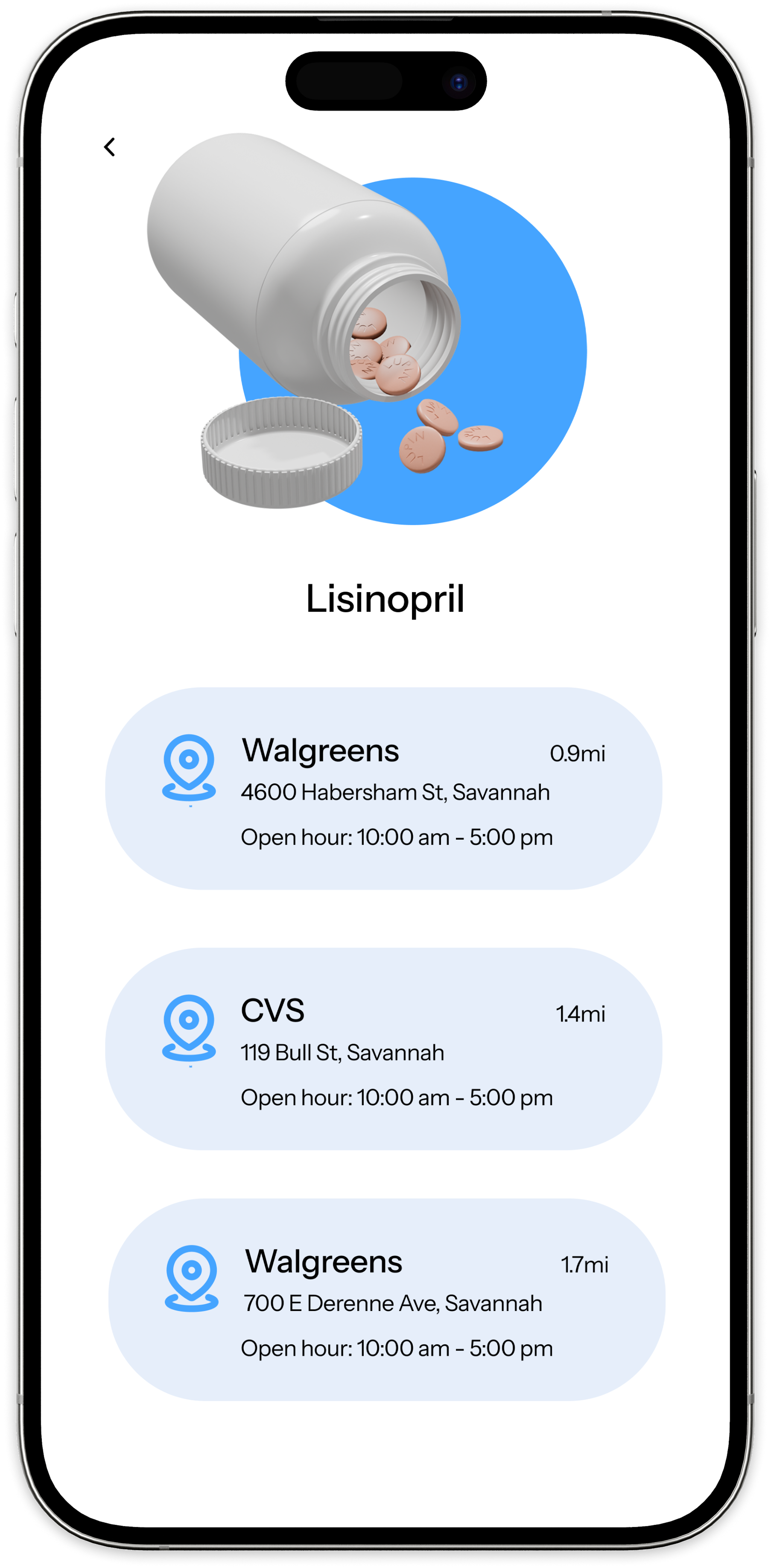
Task-based testing across three core flows: adding a medication, responding to a reminder, and finding medication information. The goal was to identify where users hesitated, what felt intuitive, and what needed clearer guidance.
Testing confirmed that the reminder confirmation flow was clear and satisfying — validating the confirmation-first model. It also exposed friction in onboarding and information discovery, reinforcing that clarity at entry points is as important as clarity in the core flow.
After completing the first round of usability testing on v1, I received structured feedback from my professor that reframed how I understood the problem. The issues weren't isolated — they pointed to a deeper misalignment between the design and the core user need.
The v1 architecture was built around medication scheduling and reminders. But the feedback made clear that the real unmet need wasn't reminding users to take their medication — it was confirming whether they actually did. No feature in v1 addressed this. The confirmation gap existed, and the structure wasn't designed to solve it.
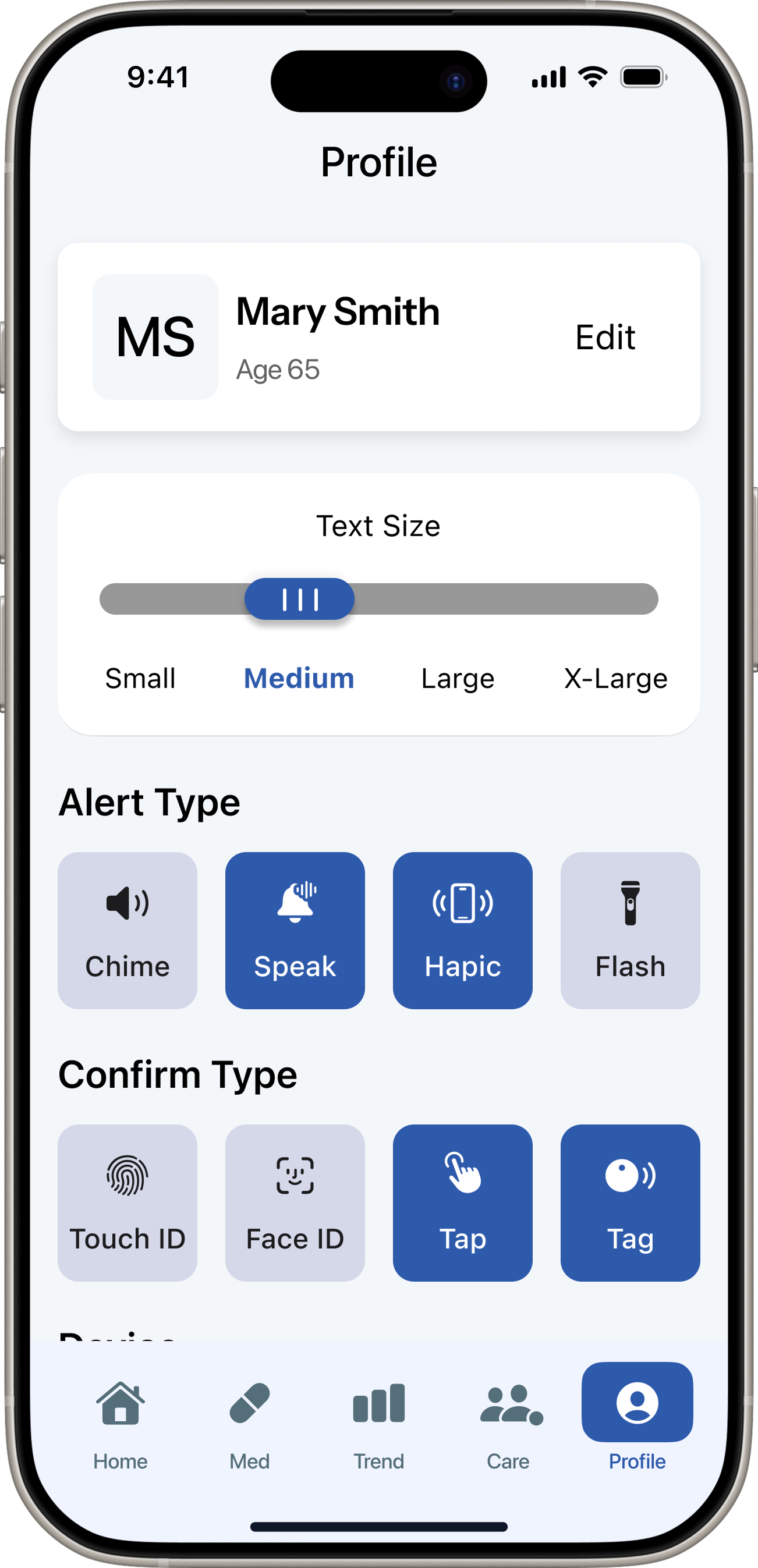
At the same time, several other problems surfaced. The information architecture organized content around medication management as a whole, which dispersed attention across too many touchpoints. For users 65+, this created unnecessary cognitive load. Accessibility was also insufficient — text sizes, contrast ratios, and touch targets didn't meet the needs of the target demographic in practice.
These weren't problems I could patch. Fixing confirmation would require making it the primary interaction — not a secondary action buried in navigation. That meant rethinking the IA from the ground up, which opened the space to introduce NFC-based physical confirmation, AI-powered adherence insights, and a multi-role ecosystem connecting patients and caregivers.
“The full redesign wasn't a setback. It was the moment the project found its real problem statement.”
Patient app — 5 tabs. Redesigned after testing exposed structural misalignment with the core user need.






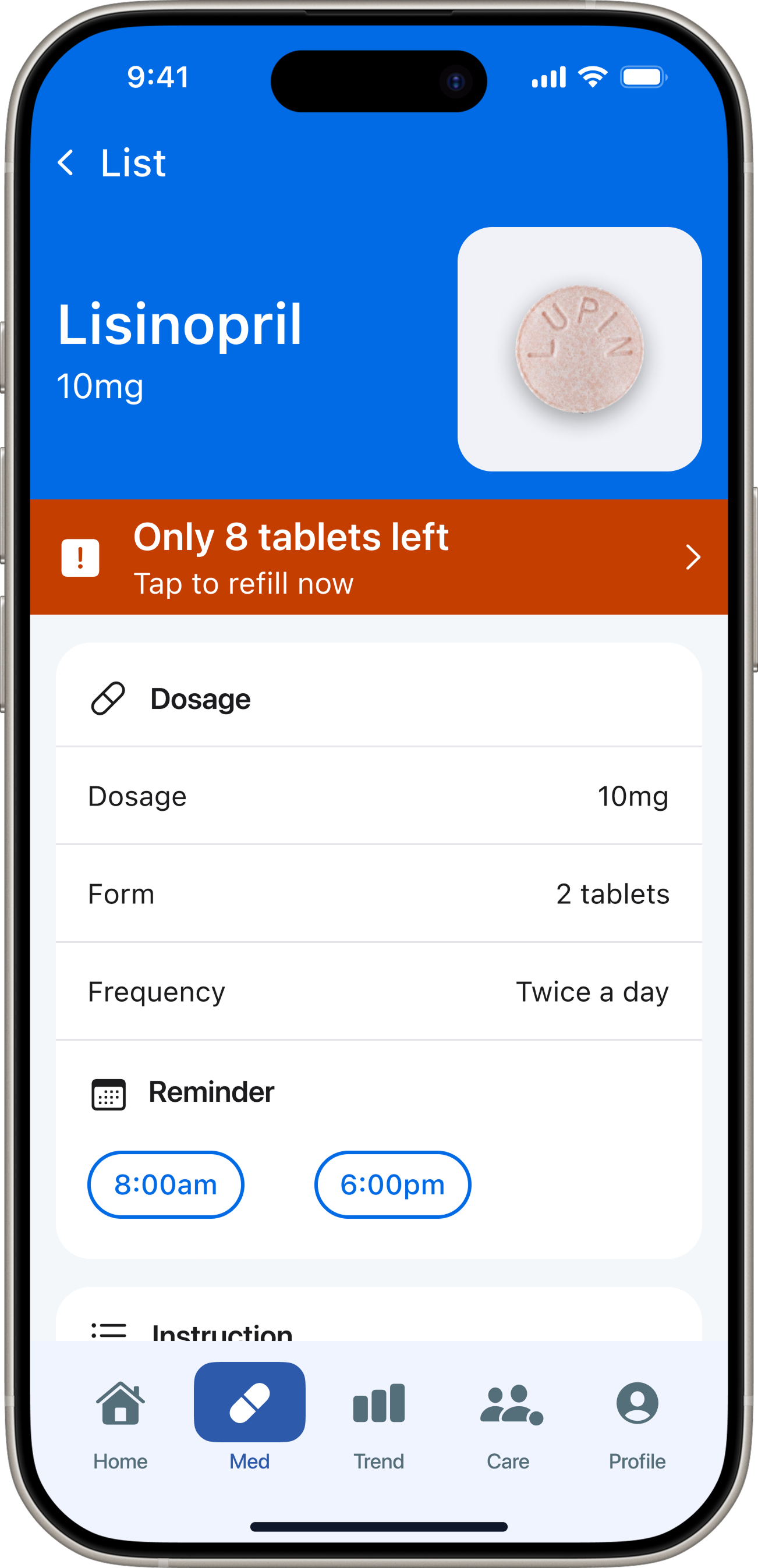
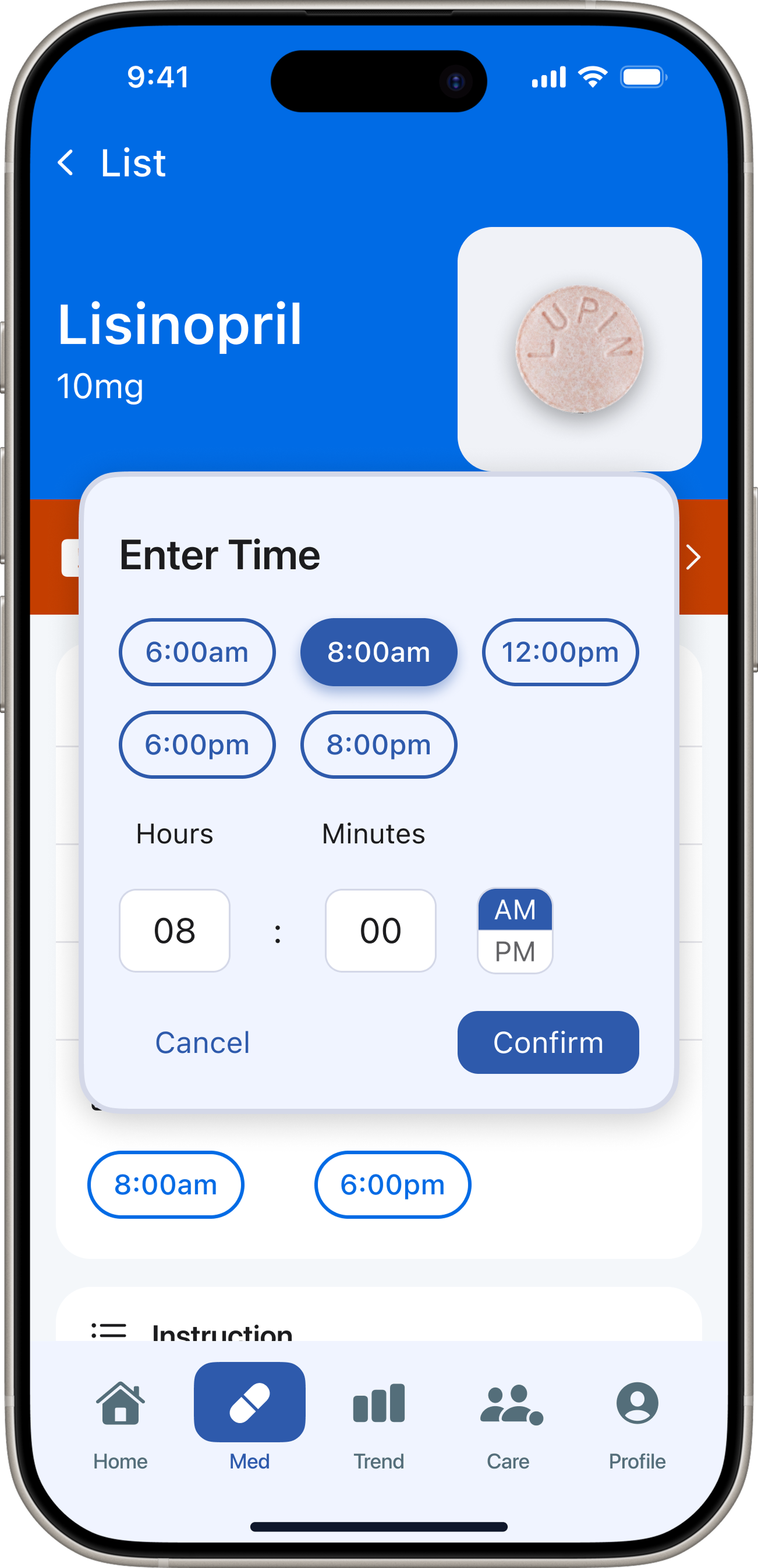
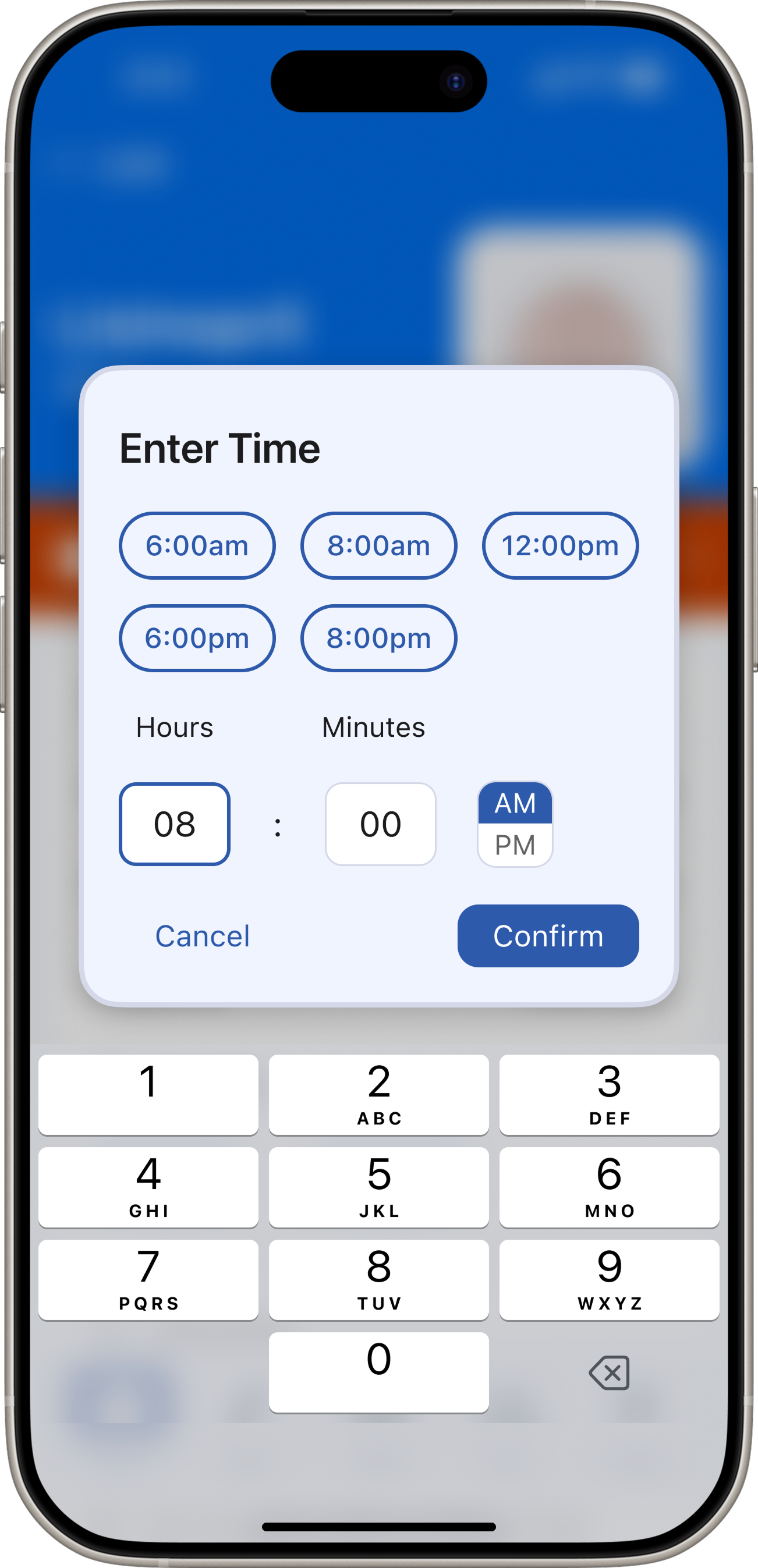
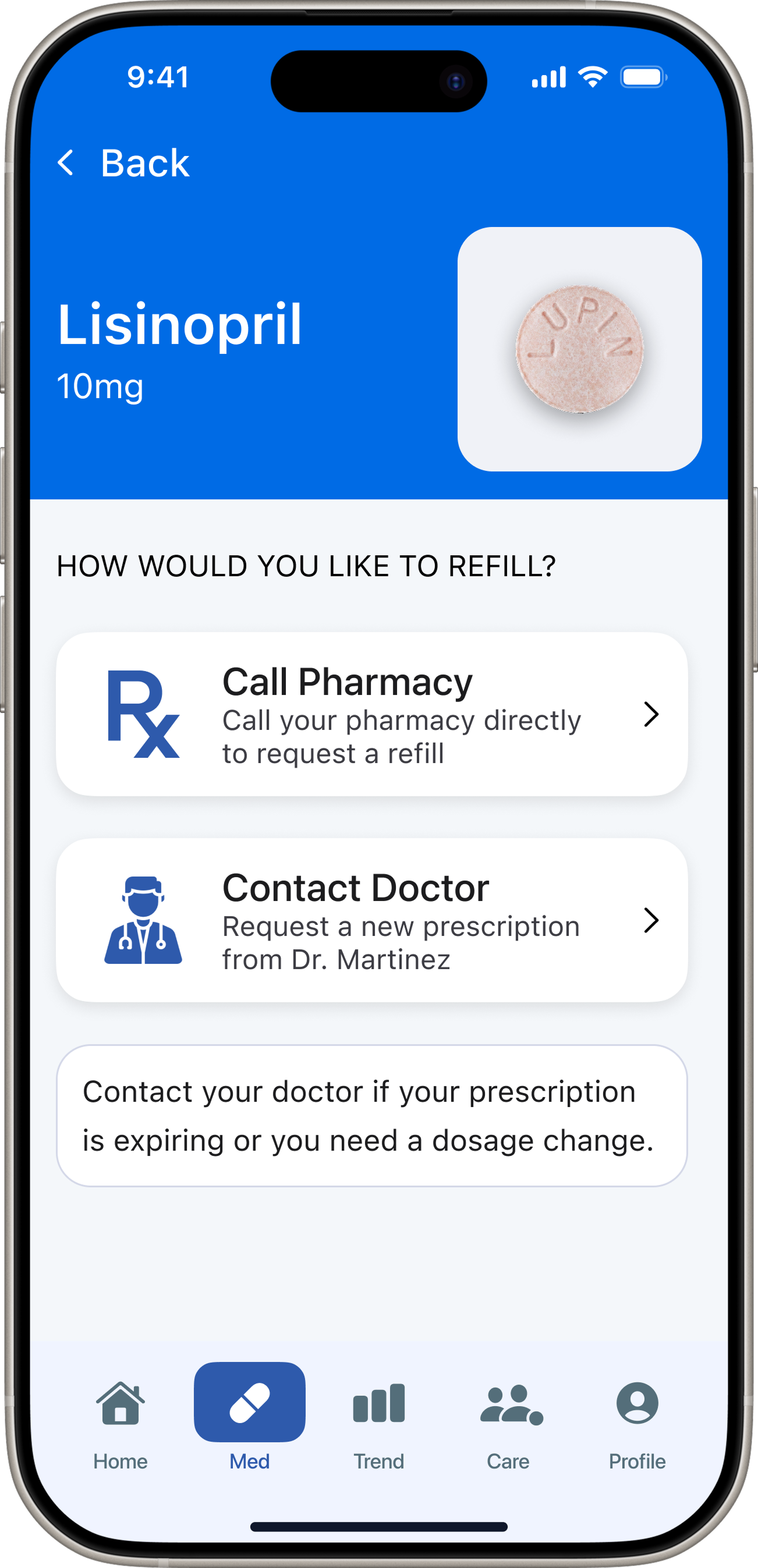

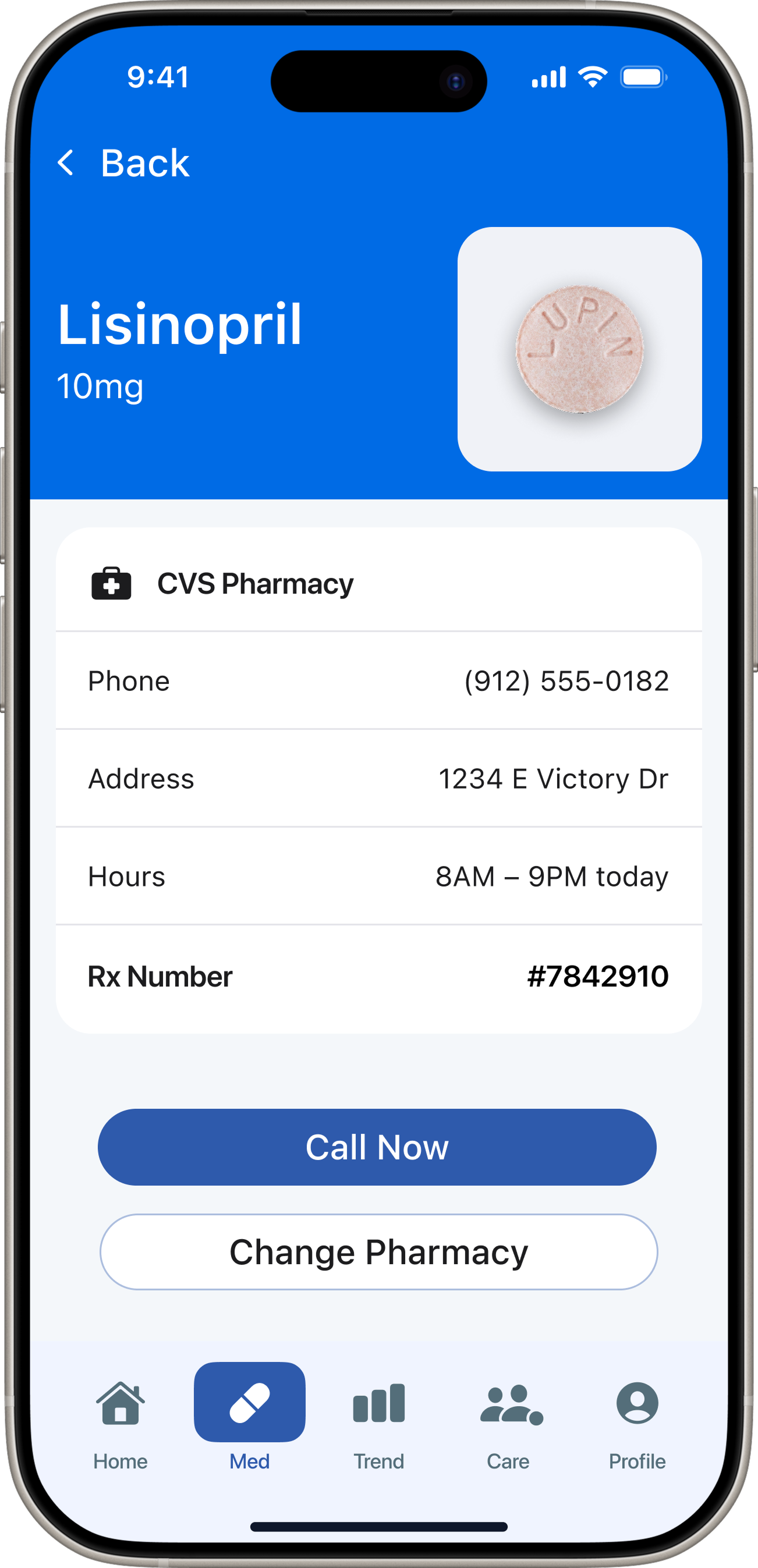
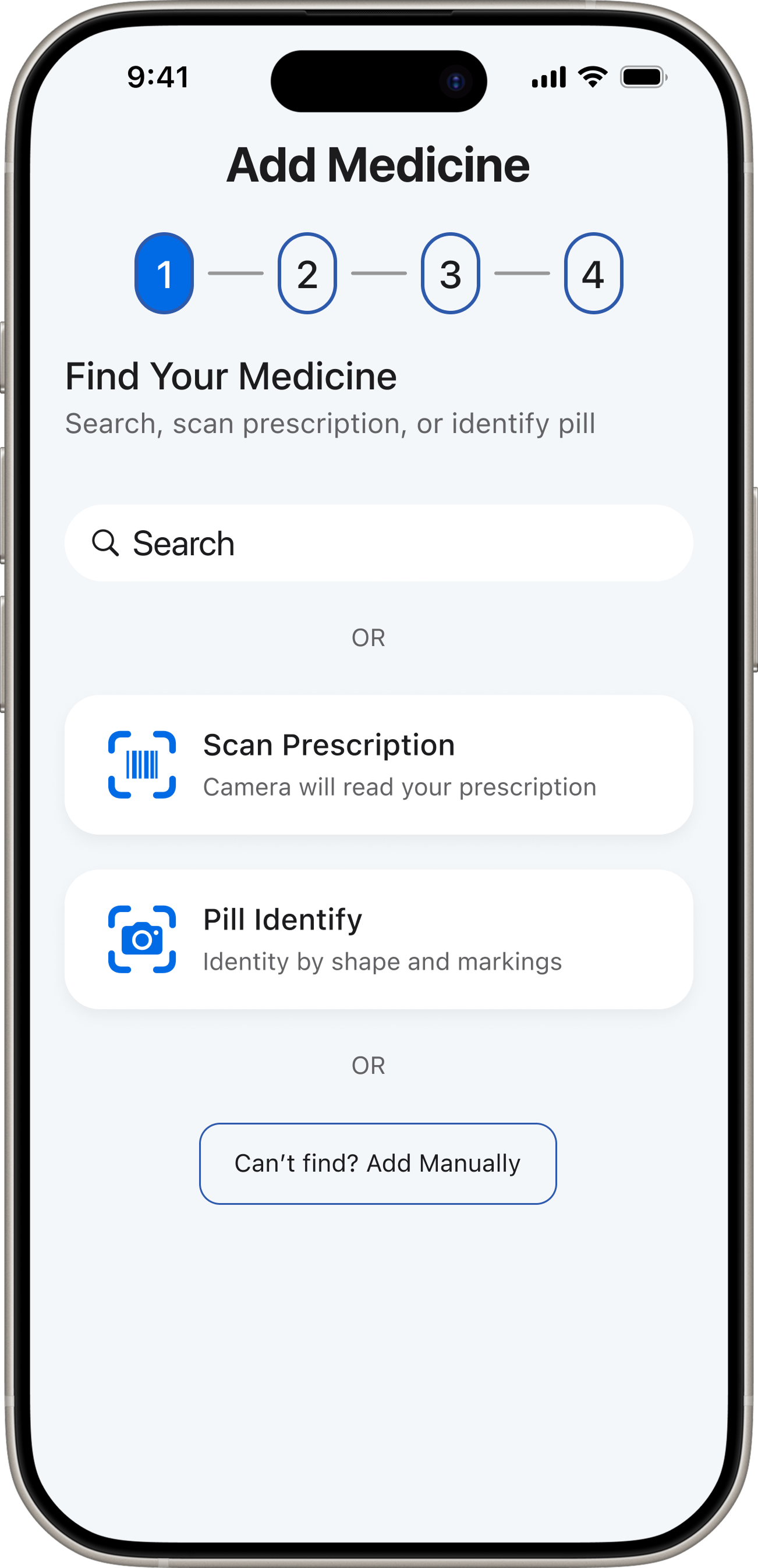
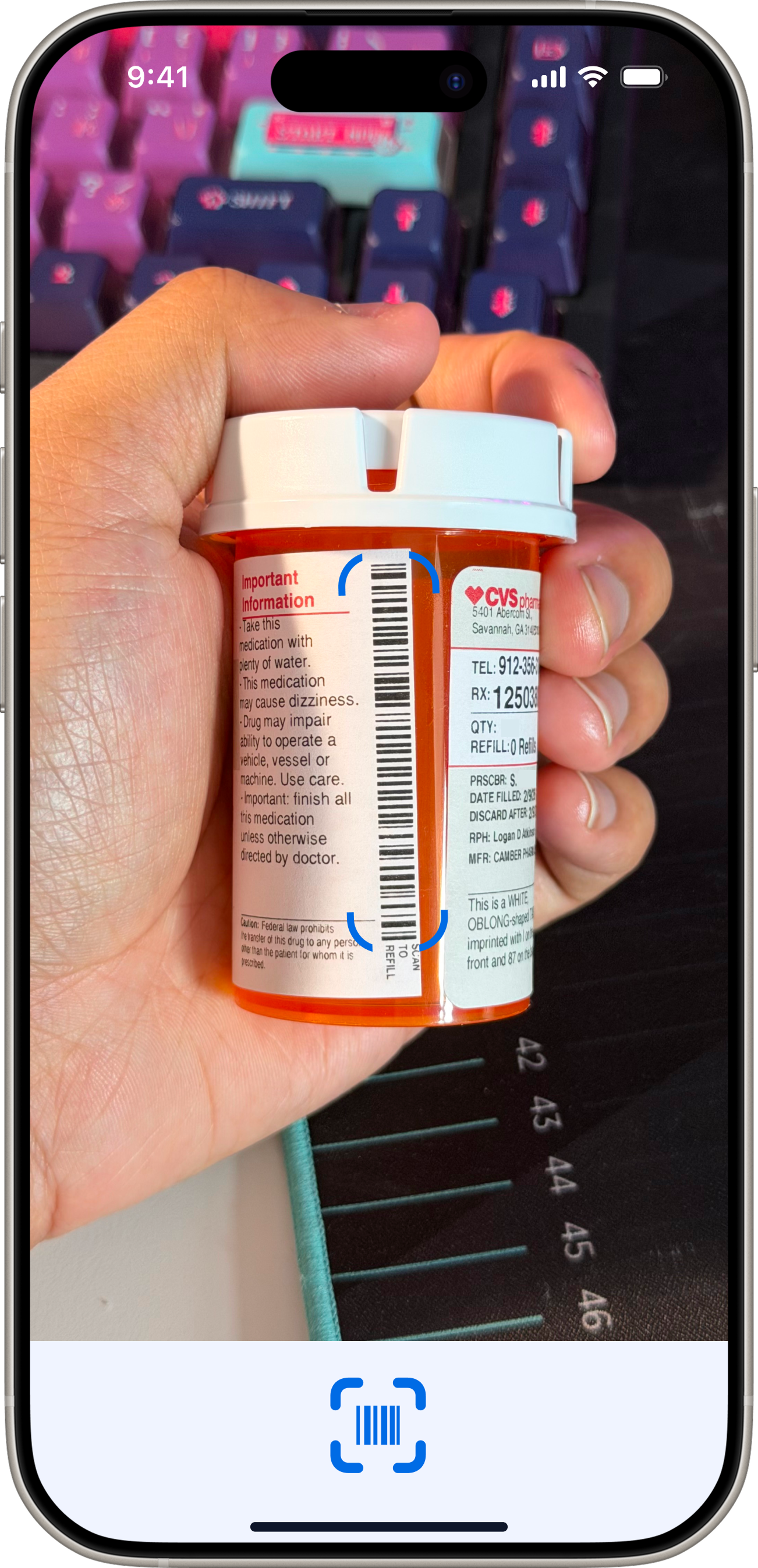
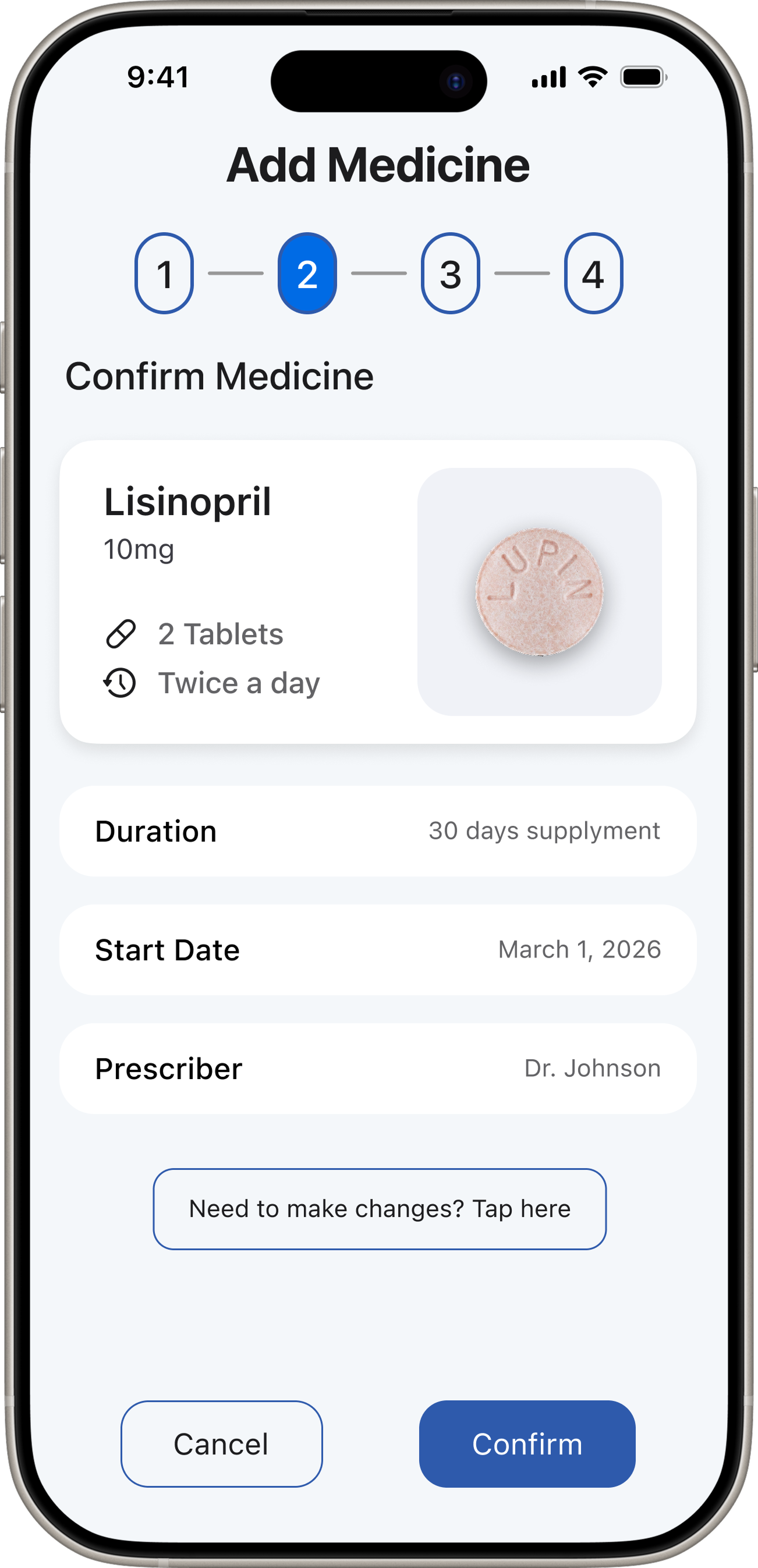

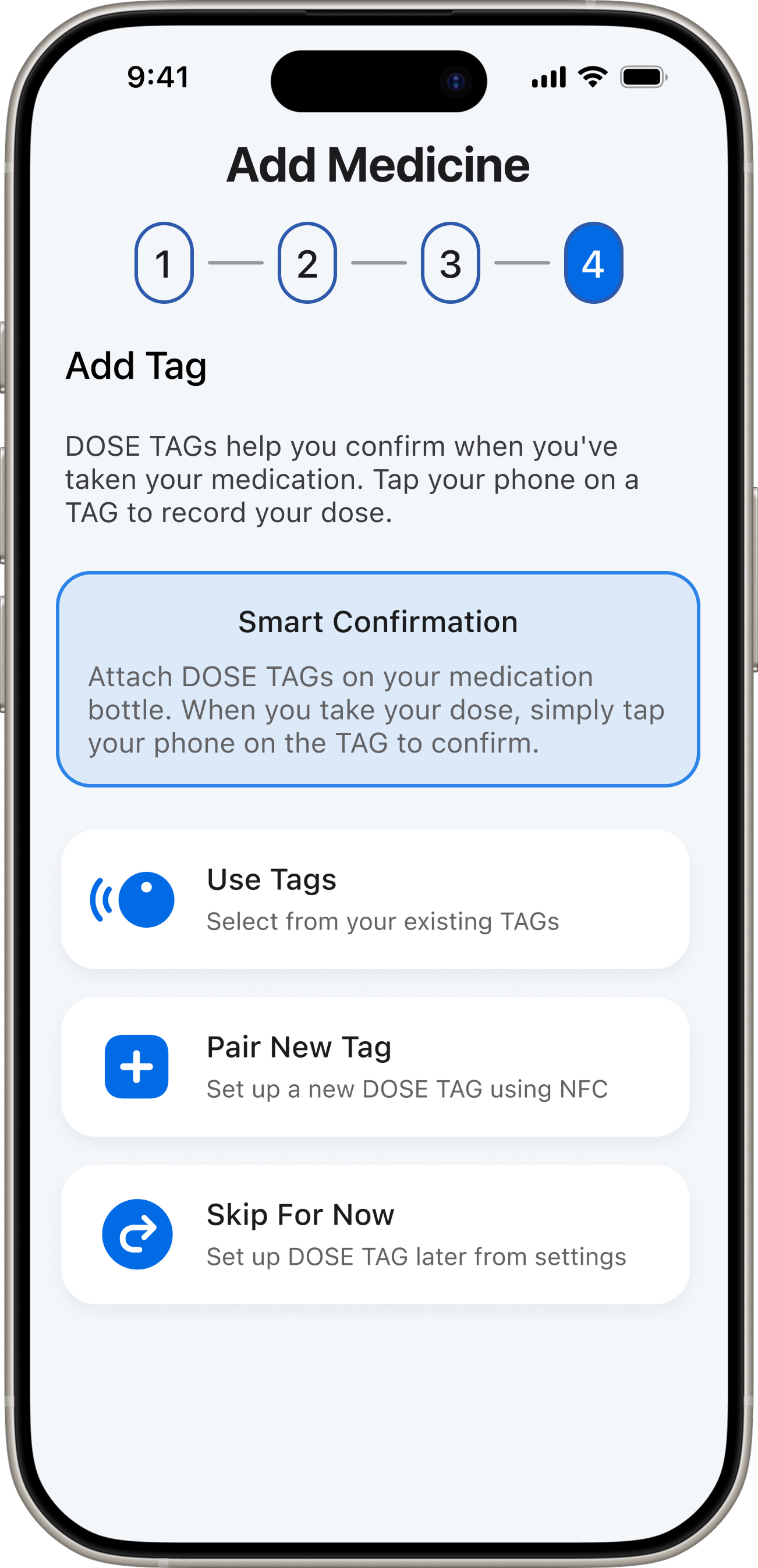
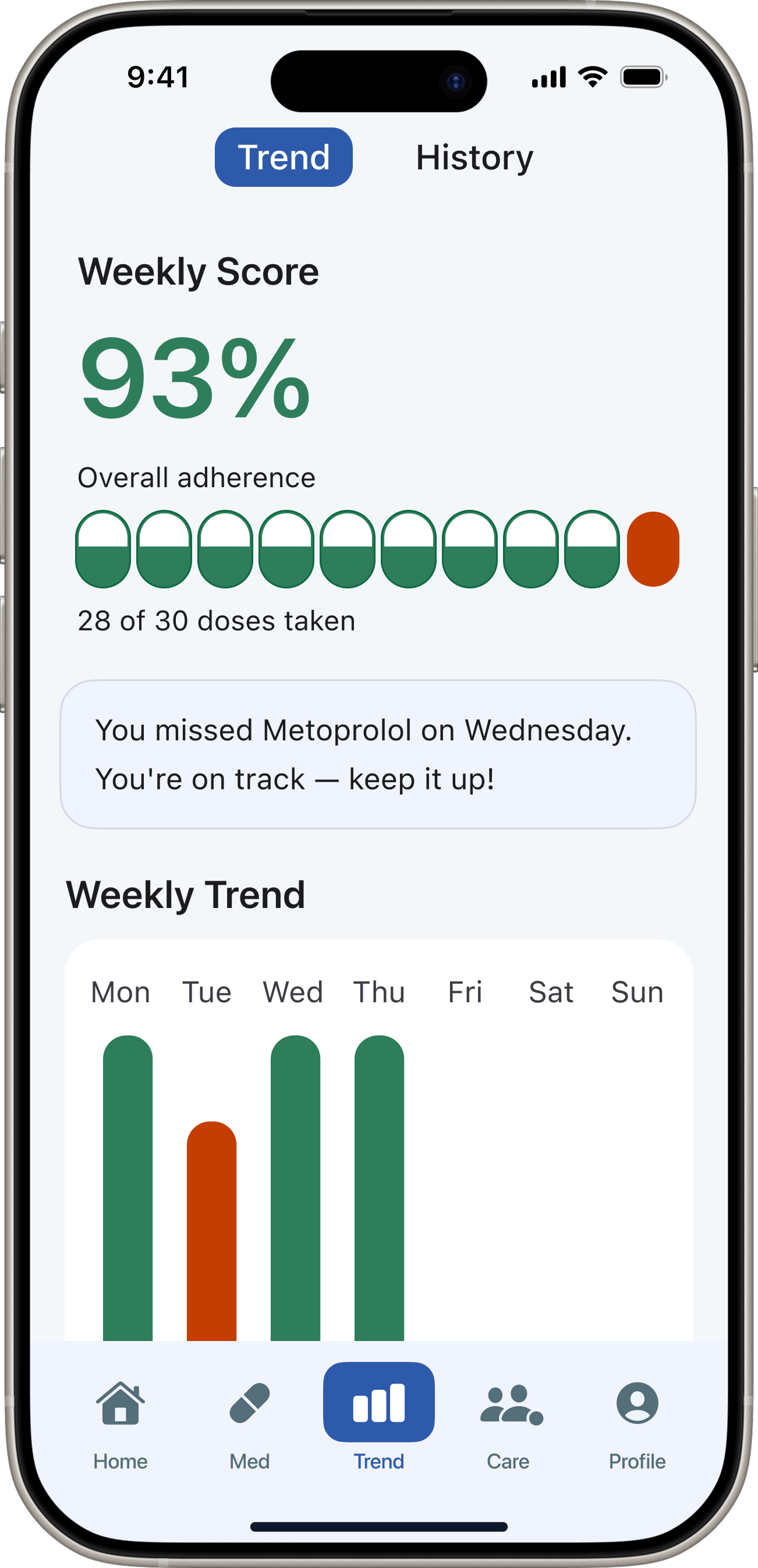
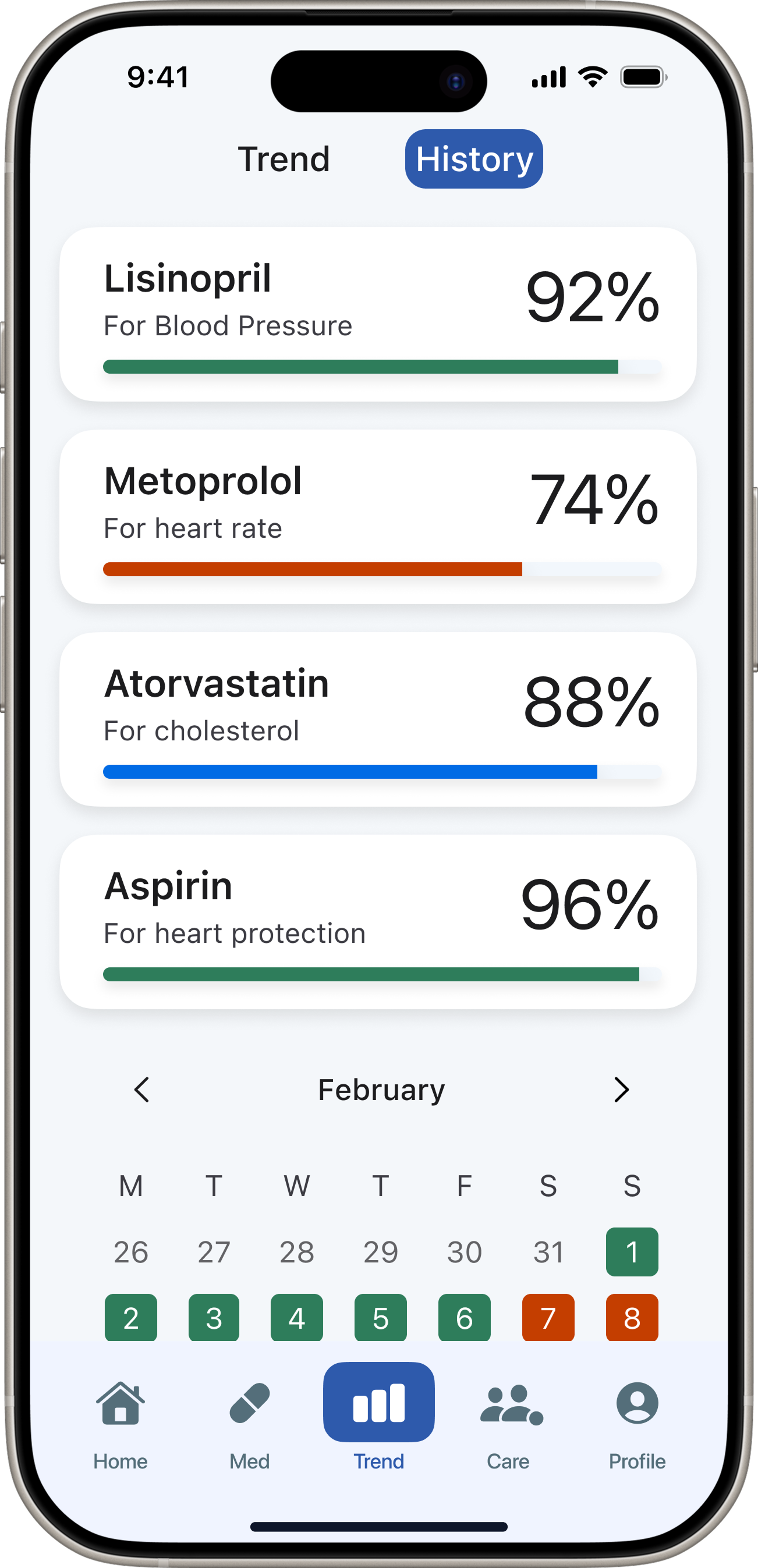
“DoseCare taught me that the best design for vulnerable users is not more features — it's relentless focus on a single core problem.”